Introduction
Worldwide trauma exposure is experienced by 69.7% of the population during life-time and 5.6% of those affected develop post-traumatic stress disorder (PTSD; Koenen et al. Reference Koenen, Ratanatharathorn, Ng, McLaughlin, Bromet and Stein2017). In PTSD, fear responses are intense and persist over time (Blechert et al. Reference Blechert, Michael, Vriends, Margraf and Wilhelm2007; Wessa & Flor, Reference Wessa and Flor2007; Jovanovic et al. Reference Jovanovic, Blanding, Norrholm, Duncan, Bradley and Ressler2009). In addition, patients suffering from PTSD respond with strong physiological reactions to cues that symbolise or resemble the traumatic event (Pole, Reference Pole2007; Hayes et al. Reference Hayes, Hayes and Mikedis2012; Parsons & Ressler, Reference Parsons and Ressler2013). This suggests an overgeneralisation of fear responses, i.e. an induction of fear by a variety of stimuli that are not directly linked to the original traumatic event. Since the pioneering work of Watson & Rayner (Reference Watson and Rayner1920), who described the generalisation of fear responses of ‘small Albert’, it is well known that the induction of fear by a wide range of diverse stimuli may cause an extreme burden and lead to an absence of the feeling of safety in every-day life (Hermans et al. Reference Hermans, Baeyens, Vervliet, Robinson, Watkins and Harmon-Jones2013). However, in contrast to many studies that reveal alterations of acquisition and extinction of fear responses in PTSD (e.g. Bremner et al. Reference Bremner, Vermetten, Schmahl, Vaccarino, Vythilingam and Afzal2005; Jovanovic et al. Reference Jovanovic, Ely, Fani, Glover, Gutman and Tone2013; Gamwell et al. Reference Gamwell, Nylocks, Cross, Bradley, Norrholm and Jovanovic2015; McLaughlin et al. Reference McLaughlin, Sheridan, Gold, Duys, Lambert and Peverill2015), experimental data on fear generalisation alterations in PTSD are sparse.
From a process-oriented perspective, overgeneralisation is based on classical fear conditioning and is conceptually best related to the ‘fear network’ (Lang, Reference Lang, Rachman and Maser1985). Here, a neutral stimulus (NS) is associated with an aversive unconditioned stimulus (US). Following this pairing, the NS elicits the conditioned fear response (CR) as a conditioned stimulus (CS+). Additional stimuli that were not present during the initial learning phase may be integrated into the fear network merely by perceptual similarities or a former association with the CS+ and as a consequence equally trigger fear responses (see also Ehlers & Clark, Reference Ehlers and Clark2000; Keane & Barlow, Reference Keane, Barlow and Barlow2002). From an evolutionary perspective, generalisation is a highly advantageous process that facilitates learning by transferring prior learning experiences to similar situations (Armony et al. Reference Armony, Servan-Schreiber, Romanski, Cohen and LeDoux1997; Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008). However, it may also hamper functioning, if fear is overgeneralised to harmless stimuli resulting in a fear network that is too broad (Hermans et al. Reference Hermans, Baeyens, Vervliet, Robinson, Watkins and Harmon-Jones2013).
The few experimental studies that have explicitly investigated fear generalisation in PTSD point to an overgeneralisation of fear in this disorder (Morey et al. Reference Morey, Dunsmoor, Haswell, Brown, Vora and Weiner2015; Kaczkurkin et al. Reference Kaczkurkin, Burton, Chazin, Manbeck, Espensen-Sturges and Cooper2016). In PTSD related to combat exposure, Kaczkurkin et al. (Reference Kaczkurkin, Burton, Chazin, Manbeck, Espensen-Sturges and Cooper2016) investigated fear responses to a danger and safety cue, as well as to stimuli with varying degrees of perceptual similarity to the danger and safety cues (generalisation stimuli). Their findings revealed stronger fear responses to generalisation stimuli in PTSD compared with trauma-exposed controls (Kaczkurkin et al. Reference Kaczkurkin, Burton, Chazin, Manbeck, Espensen-Sturges and Cooper2016). Similar preliminary findings have been reported in PTSD related to mixed traumatic events (Lissek & van Meurs, Reference Lissek and van Meurs2015).
Childhood maltreatment seems to be particularly important for fear overgeneralisation later in life: Morey e t al. (Reference Morey, Dunsmoor, Haswell, Brown, Vora and Weiner2015) identified childhood trauma as an aggravating factor in the overgeneralisation of fear in military veterans with PTSD. In general, the risk of developing PTSD in the aftermath of prolonged childhood maltreatment is not only greatly increased (e.g. US: 39.1%; Molnar et al. Reference Molnar, Buka and Kessler2001), but has also been associated with a distinct psychopathological profile. A specific diagnostic entity has been proposed and will be included in the revision of the ICD 11, i.e. complex PTSD (Maercker et al. Reference Maercker, Brewin, Bryant, Cloitre, Reed and van Ommeren2013; Shevlin et al. Reference Shevlin, Hyland, Karatzias, Fyvie, Roberts and Bisson2017). In addition to the core PTSD symptoms such as re-experiencing, avoidance and hyperarousal, the symptom pattern comprises ‘disturbances in self-organisation’, i.e. affect dysregulation, negative self-concept and interpersonal disturbances. Disturbances in self-organisation are generalised to a variety of contexts, with the potential of a detachment from the traumatic event (Hyland et al. Reference Hyland, Murphy, Shevlin, Vallieres, McElroy and Elklit2017). To date, there are no experimental studies investigating fear generalisation processes after prolonged interpersonal childhood abuse in individuals with and without PTSD.
The aim of the present study was to experimentally investigate fear generalisation in women with PTSD related to childhood abuse, since these individuals may be especially prone to developing a generalised symptom pattern. To investigate whether alterations in generalisation processes are indeed indicative of childhood abuse-related PTSD or constitute an unspecific alteration in fear processing linked to trauma exposure, we contrasted PTSD participants not only to non-trauma exposed healthy controls, but also to participants with a history of childhood abuse who have not been diagnosed with any mental disorders in their lives (trauma controls). We hypothesised (1) that an overgeneralisation of fear characterises PTSD compared with the controls, i.e. that they show stronger subjective and physiological fear responses to stimuli that are perceptually similar to a stimulus that has been previously linked to an aversive event. Moreover, we aimed at elucidating potential underlying mechanisms of overgeneralisation, by investigating whether the groups differ in basal cognitive processes such as perception and discrimination of stimulus features or in the acquisition of fear responses. We hypothesised (2) that PTSD participants differ from both healthy and trauma controls already during fear acquisition, but not in basal perception processes, and (3) that alterations during acquisition are linked to the extent of fear overgeneralisation.
Methods and materials
Sample description
Thirty female individuals meeting the criteria for PTSD related to repeated childhood abuse were matched for age and years of education to two healthy female control samples. The trauma control group (TC) consisted of 30 mentally healthy participants with a history of repeated childhood abuse. The healthy control group (HC) consisted of 30 healthy, non-trauma exposed participants. The individuals in both control groups have not been diagnosed with any mental disorders throughout their live (see also Rausch et al. Reference Rausch, Herzog, Thome, Ludascher, Muller-Engelmann and Steil2016). Enrolment was restricted to women between ages 18 and 65 years. Diagnostic and consenting procedures, as well as inclusion and exclusion criteria are included in the online Supplementary Material S1.
PTSD was diagnosed with the Structured Interview for DSM-IV (SCID-I; Wittchen et al. Reference Wittchen, Wunderlich, Gruschwitz and Zaudig1997). PTSD symptom severity was assessed using the Davidson Trauma Scale (DTS; Davidson et al. Reference Davidson, Book, Colket, Tupler, Roth and David1997), and depressive symptom severity was assessed with the Beck Depression Inventory (BDI-II; Hautzinger et al. Reference Hautzinger, Kuehner, Buerger and Keller2003). The severity of childhood traumatic experiences was measured with the Childhood Trauma Questionnaire (CTQ; Bernstein & Fink, Reference Bernstein and Fink1998). Moreover, we used the Life Events Checklist to assess the occurrence and frequency of traumatic events both before and after age 18 (National Center of Traumatic Stress; Gray et al. Reference Gray, Litz, Hsu and Lombardo2004). Sample characteristics are summarised in Table 1.
Table 1. Sample characteristics
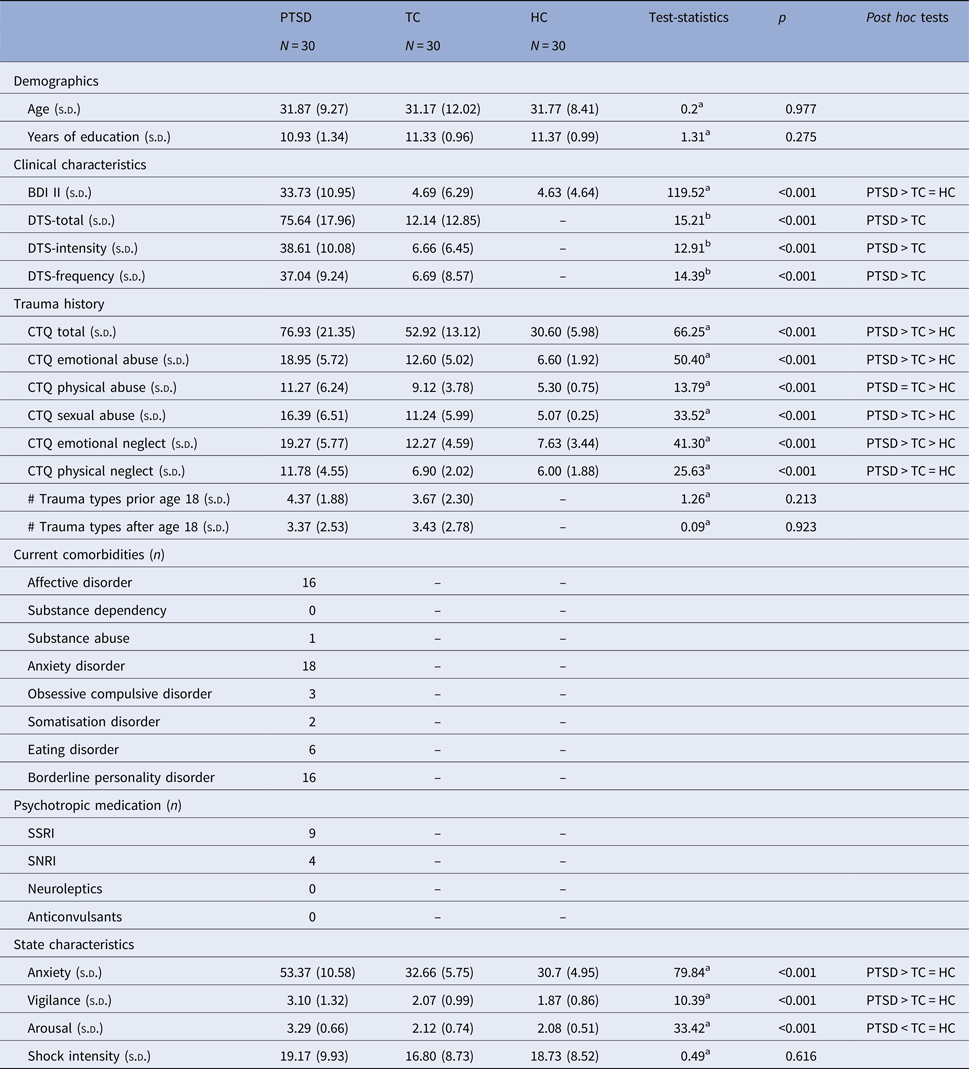
PTSD, post-traumatic stress disorder group; TC, trauma control group; HC, healthy control group; MDD, major depressive disorder; CTQ, childhood trauma questionnaire; DTS, Davidson Trauma Scale; BDI-II, Beck Depression Inventory; anxiety, State-Trait-Anxiety Inventory – State (STAI-S; Laux et al. Reference Laux, Glanzmann, Schaffner and Spielberger1981); vigilance, Stanford Sleepiness Scale (SSS; Hoddes et al. Reference Hoddes, Zarcone, Smythe, Phillips and Dement1973); arousal, Self-Assessment Manikin (SAM; Bradley & Lang, Reference Bradley and Lang1994); SSRI, selective serotonin reuptake inhibitor; SNRI, selective noradrenalin reuptake inhibitor; s.d., standard deviation; # trauma types, Life Event Checklist (National Center of Traumatic Stress; Gray et al. Reference Gray, Litz, Hsu and Lombardo2004).
Significance threshold p < 0.05.
a F-value.
b T-value.
Experimental procedure
Experimental tasks
Fear conditioning and generalisation were tested with the fear conditioning and generalisation paradigm introduced by Lissek et al. (Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008). This paradigm assesses fear responses to both conditioned danger (CS+) and safety cues (CS−), as well as to generalisation stimuli parametrically varying in similarity to the CS+ and CS−. The paradigm comprises three test phases, i.e. pre-acquisition, acquisition and generalisation.
The stimuli were comprised of 10 circles of gradually increasing size (Fig. 1c). The smallest and the largest circle served as the conditioned danger cue (CS+) and conditioned safety cue (CS−), respectively (counterbalanced across participants, Fig. 1a). The remaining eight stimuli represented the generalisation stimuli (Fig. 1c, see also online Supplementary Material S1). During testing, the stimuli were presented on a computer screen (17″ screen, stimulus duration eight seconds, Fig. 1b).

Fig. 1. Stimuli presented during different phases of the experimental paradigm together with the timing of an individual trial. (a) Stimuli presented as danger (CS+) and safety (CS−) cues during fear acquisition. (b) Timing of an individual trial exemplary for a reinforced stimulus presentation [ORR: online risk rating for the risk of the occurrence of an aversive event (US) during a time interval between 1 and 2 s following stimulus onset and until 5 s following stimulus onset; startle probe 4 or 5 s after stimulus onset; ![]() : 2 ms electrical shock 80 ms before stimulus offset during reinforced trials]. (c) Stimuli presented during generalisation testing, i.e. as danger (CS+), safety (CS−) and generalisation cue (GS). Please note, that the eight GS are combined for analyses into four generalisation classes. Please note: The assignment of the large and small circle as conditioned danger and safety cue and accordingly the generalisation was balanced across participants.
: 2 ms electrical shock 80 ms before stimulus offset during reinforced trials]. (c) Stimuli presented during generalisation testing, i.e. as danger (CS+), safety (CS−) and generalisation cue (GS). Please note, that the eight GS are combined for analyses into four generalisation classes. Please note: The assignment of the large and small circle as conditioned danger and safety cue and accordingly the generalisation was balanced across participants.
Participants were told that they were going to see several circles; some of them were sometimes followed by an electrical shock. Participants were asked to learn to predict, whether a displayed picture will be followed by an electrical shock.
During pre-acquisition, the two CSs were presented six times together with six inter-trial-intervals (ITI, fixation-cross). No stimuli were paired with an electrical shock. The pre-acquisition phase was preceded by nine startle probes to reduce initial startle reactivity (habituation).
During acquisition, the CS+ was paired with an aversive US (2 ms, electrical shock intensity was individually set to a level ‘highly uncomfortable, but not painful’, see Table 1 for shock intensities) (Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008). Overall, 12 CS+ and 12 CS− trials, as well as 12 ITIs, were presented to participants with a reinforcement rate of 75% for the CS+.
Generalisation testing started after a 5-min rest period. Participants were instructed to remember what they had learned and were informed that they were going to see the circles again. During testing, the CS+ (eight trials), CS− (eight trials), ITI (eight trials) and each of the eight generalisation stimuli (four trials) were presented in a pseudorandomised order. To prevent extinction of the CR, two of the CS+ trials were combined with an electrical shock (25% reinforcement). Generalisation testing was preceded by two startle probes to reduce initial startle reactivity (habituation).
A perceptual discrimination task was additionally conducted to assess the accuracy and speed of basal perceptional processes, i.e. the basal ability to discriminate stimuli of varying sensory similarity. During this task, each trial started with the presentation of either the CS+ or CS− (stimulus duration 2 s). Subsequently, a comparison cue was presented in the centre of the screen. Participants had to assess the similarity between stimuli on a 10-point Likert scale (1 = no similarity to 10 = high similarity). After the response, stimulus presentation was terminated and the next trial started after a variable ITI (range 1500–3000 ms, mean duration 2170 ms). Each CS (CS+/CS−) was presented 10 times and combined with the stimulus itself, the other CS and each generalisation stimulus, resulting in 20 trials.
Measurement variables
Online risk ratings, reaction time of online risk ratings (RT) and fear-potentiated startle (FPS) served as dependent measurements during all phases of the fear conditioning and generalisation paradigm (Fig. 1b).
Online risk ratings were evaluations of the risk of the occurrence of an electrical shock associated with the presented stimulus (10-point Likert scale ranging from 1 = no risk, to 10 = high risk). To indicate their responses, subjects had to move a red dot from a starting area to one of 10 target areas, which were displayed at equal distance from the starting area. RTs were defined as the time between reaching the target area and leaving the starting area. RTs served as an index of uncertainty during the risk judgements as proposed by Lissek et al. (Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008, Reference Lissek, Rabin, Heller, Lukenbaugh, Geraci and Pine2010, Reference Lissek, Kaczkurkin, Rabin, Geraci, Pine and Grillon2014), with higher RTs suggesting higher uncertainty. The shape of the RT distribution depending on the stimulus types is formed by a linear, quadratic and cubic component (Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008). Lissek et al. (Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008, p. 684) suggested that RT captures the ‘threat ambiguity’ of a presented stimulus, with ‘faster risk ratings for stimuli with unambiguous safe/threat information (CS+, CS−) and slower RT for stimuli with more uncertain signal value’, which is indicated by the quadratic component (see also Lissek et al. Reference Lissek, Rabin, Heller, Lukenbaugh, Geraci and Pine2010, Reference Lissek, Kaczkurkin, Rabin, Geraci, Pine and Grillon2014). Moreover, RT becomes slower with increasing similarity of a stimulus to the threat-associated cue (linear component), since the differentiation between stimuli and the associated risk of an aversive event becomes more demanding and the judgement becomes uncertain (Lissek et al. Reference Lissek, Kaczkurkin, Rabin, Geraci, Pine and Grillon2014). In line, a smaller linear slope indicates a lower differentiation between stimuli when judging risk, i.e. a stronger generalisation of the risk of threat.
FPS was measured as the potentiated eye-blink startle reflex to a loud noise [40 ms, 95 dB(A)] by electromyography of the orbicularis oculi muscle. To measure FPS, CS and generalisation stimuli were followed after 4 or 5 s by acoustic startle probes. Additionally, a similar number of startle probes was presented during ITIs. For further details, see online Supplementary Material S1.
According to previous studies, online risk ratings and FPS were assessed in separate trials (50% of trials) since startle response may be influenced by simultaneous ratings due to attentional demands or movement preparation (Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008).
Statistical analyses
For the fear conditioning and generalisation paradigm, dependent variables were averaged separately for each experimental phase and stimulus type. Measurement variables of generalisation stimuli were further combined for two consecutive levels of similarity each, resulting in four generalisation classes [Fig. 1c, online Supplementary Material S1, see also (Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008)]. Mean FPS, online risk ratings and RT were analysed separately for each task with repeated measure variance-analytical designs (rmANOVA). All designs comprise the between-participants factor ‘group’ (PTSD, TC, HC) and the experimental factor ‘stimulus type’. For pre-acquisition and acquisition phases, this resulted in a 3 × 2 rmANOVA with CS+ and CS− as the factor ‘stimulus type’. For further description of the effects in the ANOVA designs, post hoc comparisons were done by sub-designs of ANOVA design and/or pairwise comparisons (Bonferroni-adjusted for multiple testing). For generalisation testing, the design was extended by the generalisation classes as additional levels of the factor ‘stimulus type’ resulting in a 3 × 6 rmANOVA. In the case of a significant influence of the factor ‘stimulus type’, we further described the nature of this effect through trend analyses. Here, we analysed the linear, quadratic and cubic components of the shape of the RT distribution along the continuum of stimulus types (ranging from safety to danger cue). Thereby, we used the advantage of the parametrically varied levels of this factor. If trend analyses revealed differences between groups, we compared the coefficients of the concerned component pairwise between groups (Bonferroni-corrected for multiple testing).
Similarity ratings and RT during the perceptual discrimination task were analysed with a 3 × 2 × 6 rmANOVA with the between-subjects factor ‘group’, and the within-subject factors ‘reference’ (CS+, CS−) and ‘comparison stimulus’ (CS+, CS−, class 1–4).
To explore covariation of alterations in fear generalisation with alterations of perceptual discrimination, fear responses during baseline, fear acquisition, and the severity of childhood maltreatment and PTSD symptomatology, Pearson's correlation coefficients were calculated. Because of the exploratory nature of these analyses, we did not correct for multiple comparisons to avoid an inflation of type II error. Consequently, the findings must be interpreted taking the inflation of type I error into account.
Since single participants had to be excluded from the statistical analyses, sample sizes were reduced as follows (for details on exclusion criteria, please see online Supplementary Material S1): N for online risk ratings: pre-acquisition: HC = 30, TC = 27, PTSD = 29, acquisition: HC = 29, TC = 29, PTSD = 30, generalisation: HC = 29, TC = 29, PTSD = 29; for RT: pre-acquisition HC = 30, TC = 27, PTSD = 29, acquisition/generalisation: HC = 30, TC = 29, PTSD = 30; and for FPS: pre-acquisition HC = 26, TC = 27, PTSD = 27, acquisition/ generalisation: HC = 23, TC = 27, PTSD = 27.
Statistical significance was set to p < 0.05. Effect sizes were calculated as Cohen's d. All analyses were performed using SPSS (IBM SPSS Statistics for Windows, Version 23.0, Armonk, NY: IBM Corp).
Results
Fear conditioning and generalisation paradigm
Pre-acquisition
Online risk ratings differed between groups (F 2,83 = 8.96, p < 0.001; Table 2a): PTSD participants rated the risks higher compared with both HC and TC participants (PTSD: 4.43, s.d. = 2.01; HC: 2.50, s.d. = 1.47; TC: 3.14, s.d. = 1.82; PTSD v. HC: p < 0.001; PTSD v. TC: p = 0.024). No difference was found between TC and HC (p = 0.536). Online risk ratings did not differ between stimulus types (F 1,83 = 0.75, p = 0.388; group x stimulus type: F 2,83 = 1.14, p = 0.326). Neither RT nor FPS differed between groups or stimulus types (Table 2a).
Table 2. Results of the analyses of variance for mean online risk ratings (ORR), reaction times (RT) and fear potential startle magnitudes (FPS) in the different phases of the experimental task.(a) Pre-acquisition, (b) fear acquisition and (c) fear generalisation for mean ORR, RT and FPS

df, degrees of freedom; d, Cohen's d.
Significance threshold *p < 0.05.
Acquisition
Online risk ratings differed between groups independent of the stimulus type (F 2,85 = 5.33, p = 0.007; group x stimulus type: F 2,85 = 0.42, p = 0.661; Table 2b, Fig. 2): PTSD participants rated the risk higher compared with HCs (p = 0.005) but not to TC individuals (p = 0.462). There was no difference between TC and HC (p = 0.224). In general, participants reported higher risk expectation for the CS+ compared with the CS−, suggesting successful fear conditioning (F 1,85 = 492.96, p < 0.001).

Fig. 2. Online risk ratings (ORR) (1), reaction times (RT) (2), fear potentiated startle magnitudes (FPS) (3) for each group regarding fear acquisition (a) and fear generalisation (b) for healthy controls (HC), trauma controls (TC) and PTSD patients (PTSD). (a1). PTSD participants expected more risk, independent of the presented stimulus type compared with HC participants. (a2) PTSD and TC participants responded faster to the danger cue and slower to the safety cue, while this pattern was reversed in HC participants. (a3) PTSD participants exhibited lower FPS to the danger cue compared with HC participants. (b1) PTSD participants expected more risk, independent of the presented stimulus type compared with HC, and on marginally significant level compared with TC participants. (b2) HC participants were characterised by a stronger increase in reaction times from the safety cue across the generalisation cues to the danger cue compared with PTSD patients, suggesting less differentiation between generalisation stimuli in PTSD, i.e. alterations in generalisation processes. (b3) No group-related effects have been observed. +: CS+; −: CS−; 1–4: generalisation class 1–4, GS = generalisation stimuli.
RTs differed between groups depending on the stimulus type (F 2,86 = 11.92, p < 0.001; Table 2b, Fig. 2). The RT of both PTSD and TC participants differed from HC, but not between PTSD and TC (2 × 2 ANOVA sub-design: group x stimulus type: PTSD v. HC: F 1,58 = 20.69, p < 0.001; TC v. HC: F 1,57 = 12.37, p = 0.001; PTSD v. TC: F 1,57 = 0.99, p = 0.325). Responses to the CS− were slower in PTSD (p = 0.003) and on marginally significant level in TC compared with HC (p = 0.064). In contrast, no group differences in RT to the CS+ were found (all p > 0.205). Comparing RTs between stimulus types revealed that PTSD and TC participants responded more slowly to the CS− compared with the CS+ (PTSD: p < 0.001; TC: p = 0.018). In contrast, HC responded faster to the CS− compared with the CS+ (p = 0.007).
FPS differed between groups depending on the stimulus type (F 2,75 = 4.39, p = 0.016; Table 2b, Fig. 2). Post hoc analyses revealed that FPS to the CS+ was reduced in PTSD compared with HC (2 × 2 ANOVA sub-design: group x stimulus type: PTSD v. HC: F 1,49 = 7.86, p = 0.007; CS+: p = 0.018; CS−: p = 0.585). In contrast, no differences were observed between PTSD and TC or TC and HC (2 × 2 ANOVA sub-design: group x stimulus type: PTSD v. TC: F 1,52 = 2.29, p = 0.136; HC v. TC: F 1,49 = 2.49, p = 0.121). In general, FPS to the CS+ was higher compared with the CS− (F 1,75 = 50.65; p < 0.001), suggesting successful fear conditioning.
Generalisation test
Online risk ratings differed between groups (F 2,84 = 4.19, p = 0.018; Table 2c, Fig. 2): PTSD individuals demonstrated heightened risk irrespective of the stimulus type compared with HC (p = 0.029), and on a marginally significant level to TC (p = 0.064), while TC did not differ from HC participants (p = 1.000). In general, participants differentiated between stimulus types; however, stimulus types did not differentially affect online risk ratings between groups (stimulus type: F 5420 = 253.05, p < 0.001; stimulus type x group: F 10420 = 1.44, p = 0.162). Trend analyses revealed a significant linear (F 1,84 = 563.81, p < 0.001) and quadratic component (F 1,84 = 100.76, p < 0.001). For further details on pairwise comparisons, see online Supplementary Material S2.
RT differed between groups depending on the stimulus type (F 10430 = 1.85, p = 0.050; Table 2c, Fig. 2). Trend analyses revealed that this difference is linked to the linear component of the shape of the relationships between the speed of risk ratings and the increasing similarity from the safety cue across the different generalisation classes to the danger cue (F 2,86 = 4.44, p = 0.015). The comparison between groups revealed a stronger increase in RT in HC compared with PTSD (β HC = 69.0, s.d. 94.7; β PTSD = 7.2, s.d. 76.6, p = 0.015), while no significant differences between TC (β TC = 24.9, s.d. 75.0) compared with PTSD (p = 1.000) and HC (p = 0.132) were found. Note however, that without a Bonferroni correction for multiple testing, the slope in TC is significantly smaller than in HC (p = 0.044). In general, there are additional significant quadratic and cubic components of the shape of the RTs across stimulus types (quadratic: F 1,86 = 27.84, p < 0.001; cubic: F 1,86 = 11.05, p = 0.001). However, these components did not differ significantly between groups (quadratic: F 2,86 = 1.66, p = 0.197; cubic: F 2,86 = 1.15, p = 0.321). For further details on pairwise comparisons see online Supplementary Material S2.
FPS did not differ between groups, either in general (F 2,74 = 0.05, p = 0.955; Table 2c, Fig. 2) or depending on the stimulus type (F 10370 = 0.564, p = 0.844). FPS differed depending on the stimulus types (F 5370 = 18.86, p < 0.001). Trend analyses revealed a significant linear component (stimulus type: F 1,74 = 92.39, p < 0.001; stimulus type x group F 2,74 = 1.33, p = 0.270). For further details on pairwise comparisons, see online Supplementary Material S2.
Perceptual discrimination task
An assessment of the level of similarity between stimuli and the RT of these assessments did not differ between groups, either in general or depending on the stimuli presented (all p > 0.166). For further details, see online Supplementary Material S2 and Table S1.
Correlation of alterations in generalisation with baseline responses, and responses during fear acquisition
To explore whether group-related alterations during generalisation testing, i.e. increased stimulus-independent online risk ratings, and the linear trend in RT are related to alterations during other cognitive processes (i.e. fear responses during pre-acquisition and acquisition), correlations were calculated separately for each group (for correlation coefficients and group statistics, see Table 3). Higher online risk ratings during generalisation testing were linked to higher online risk ratings during acquisition in all groups and during pre-acquisition in HC, but only on a marginally significant level in TC and PTSD (Table 3). Moreover, higher online risk ratings during generalisation were linked to a lower differentiation between CS+ and CS− during fear acquisition in FPS response in PTSD (Table 3), and regarding the RT response in HC (Table 3). A stronger increase in RT across stimulus types was related to lower online risk ratings and reduced differences in FPS during fear acquisition in PTSD and a reduced difference in RT during fear acquisition in HC. A comparison of correlation coefficients between groups suggests a differential relation only in regard to the association between the height of the online risk ratings during generalisation and the RT difference between safety and danger cues during fear acquisition between PTSD and HC (Table 3).
Table 3. Correlation of alterations in generalisation with baseline responses, as well as responses during fear acquisition, and clinical measurements

PTSD, post-traumatic stress disorder group, TC, trauma control group; HC, healthy control group; CTQ, childhood trauma questionnaire; DTS, Davidson Trauma Scale; RT, reaction time; FPS, fear-potentiated startle; ORR, online risk ratings.
*Significance threshold p < 0.05, †p < 0.1; °difference: safety – danger cue.
Correlation of alterations in generalisation with trauma severity
Alterations in online risk ratings and RTs during generalisation testing were not significantly related to the severity of childhood traumatisation or PTSD symptomatology (Table 3).
Discussion
The present study investigated whether patients with PTSD after exposure to repeated childhood abuse are characterised by an overgeneralisation of fear. Indeed, our findings support alterations in generalisation-related processes in PTSD depending on the domains of outcome measures. Reaction times as an index of uncertainty about the threat associated with a cue suggest a reduced differentiation across the continuum of cues from safety to danger in PTSD. Generalisation of the explicitly assessed threat risk and the linked physiological responses were not altered in those with PTSD. However, independent of generalisation processes, PTSD individuals assessed the risk for aversive events as higher, pointing to difficulties in establishing a feeling of safety. Differences between trauma control participants and both PTSD participants and healthy controls were inconclusive for many outcome measures. Our findings suggest that in trauma controls, alterations partly mirror those observed in PTSD, however, in an attenuated manner, which prevents confirmation with statistically sufficient unambiguousness.
Generalisation of fear in PTSD
Overgeneralisation is the spreading of fear to stimuli that bear a similarity to the danger cue, i.e. generalisation stimuli. We applied a fear conditioning and generalisation paradigm (Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008) and our findings confirm alterations in processes linked to the generalisation of fear in PTSD related to childhood abuse. These alterations are not revealed by how strongly an aversive event is expected within a specific stimulus context, but by alterations regarding the uncertainty with which people achieve this judgement: Depending on the specific cues, PTSD participants differed from healthy controls in processing times during risk evaluations, but not in the evaluation of the level of risk itself or the evoked startle response. Our findings revealed in healthy controls a slowing of reaction times with increasing similarity of a stimulus to the danger cue, i.e. a higher uncertainty during risk judgements due to higher demands on the differentiation from the danger cue. This slowing across stimulus types was markedly reduced in the PTSD group. It seems worth noting that in the context of generalisation stimuli the meaning of slower reaction times changes across the continuum from safety to danger. Slower reaction times for stimuli more similar to the danger cue suggest low generalisation of fear since participants are able to differentiate the perceptual features of the actual stimulus and the danger cue, but they are more uncertain about the prediction of risk (see Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008, Reference Lissek, Rabin, Heller, Lukenbaugh, Geraci and Pine2010, Reference Lissek, Kaczkurkin, Rabin, Geraci, Pine and Grillon2014). In contrast, slower reaction times for stimuli more similar to the safety cue point to overgeneralisation, i.e. feeling more uncertain about safety. Consequently, an overgeneralisation of fear is reflected in small differences in reaction times between stimulus classes, i.e. an attenuated increase in reaction times for stimuli most similar to the danger cue since a potential threat is readily noticed, and slower reaction times for stimuli similar to the safety cue when an individual is not sure about the safety linked to a stimulus. Following this reasoning, the attenuated slowing of reaction times across the stimulus types in the PTSD group points to a ‘threat ambiguity’, which is comparable across the range of stimuli presented (Lissek et al. Reference Lissek, Biggs, Rabin, Cornwell, Alvarez and Pine2008, Reference Lissek, Rabin, Heller, Lukenbaugh, Geraci and Pine2010, Reference Lissek, Kaczkurkin, Rabin, Geraci, Pine and Grillon2014). It has to be kept in mind that we found no differences in the level of reaction times in general between PTSD participants and healthy controls. This suggests that neither group can be characterised as more uncertain about their judgements independently of the signal value of a cue. Similarly, the modulation of reaction times by pure perceptual ambiguity seems to be comparable between both groups: In both groups, an inverted U-curve mirrored the variations in ambiguity due to variations in the similarity of perceptual features between a specific stimulus and the two stimuli representing the extremes of the continuum, i.e. the safety and the danger cue. In line, we found no difference between the PTSD group and HC in the quadratic component of the reaction time distribution reflecting this inverted U-curve. In summary, our data suggest that the generalisation of the explicitly assessed level of risk is not affected in PTSD, but the uncertainty with which the risk of threat is judged is affected.
It is important to note that Kaczkurkin et al. (Reference Kaczkurkin, Burton, Chazin, Manbeck, Espensen-Sturges and Cooper2016) applied a comparable paradigm in combat-exposed participants with and without PTSD. Similar to the present study, their findings suggested stronger generalisation of fear in PTSD participants. However, in contrast to our study, alterations in generalisation processing were revealed for the explicitly assessed level of risk and brain responses, while reaction times were not reported. Because of the different outcome measures as well as the different types and timing of traumatisation, the comparability of both studies is limited. Further studies are required to investigate whether differences in type and timing of traumatisation might affect different aspects of generalisation processing.
Risk perception during fear processing in PTSD
Beyond these findings on processes linked to the generalisation of fear, PTSD participants differed from healthy subjects independent of generalisation. Particularly, risk expectation was increased in the PTSD group independent of the type of stimuli presented, i.e. unrelated to the generalisation processes. A stimulus-independent higher risk expectation during generalisation testing is in line with preliminary findings by Lissek et al. in PTSD with a history of various trauma types (reported in a review article, see Lissek & van Meurs, Reference Lissek and van Meurs2015). These authors discussed their findings as a reflection of sensitisation processes. Sensitisation represents a non-associative learning mechanism, in which fear is elicited when confronted with novel cues by an activation of the fear system in response to an aversive event (Marks & Tobena, Reference Marks and Tobena1990). In contrast to generalisation, these novel cues are not necessarily related to the aversive event (Maier & Watkins, Reference Maier and Watkins2005). This interpretation is in line with the heightened risk expectation in PTSD participants already present during baseline testing and fear learning in the present study. However, the differentiation between generalisation and sensitisation requires an experimental paradigm extended by additional stimuli that clearly diverge from the danger cue. By applying this approach in veterans with and without PTSD, Kaczkurkin et al. (Reference Kaczkurkin, Burton, Chazin, Manbeck, Espensen-Sturges and Cooper2016) demonstrated that the CR did not generalise from the danger cue to a novel control stimulus, suggesting that the observed effects of overgeneralisation are not due to sensitisation processes.
Alterations in fear learning in PTSD
It seems worth mentioning that the concept of fear overgeneralisation in PTSD literature was driven by the idea that reduced discrimination between danger and safety cues during fear learning represents a form of overgeneralisation (e.g. Grillon & Morgan, Reference Grillon and Morgan1999; Jovanovic et al. Reference Jovanovic, Norrholm, Blanding, Davis, Duncan and Bradley2010; Davis et al. Reference Davis, Jovanovic, Norrholm, Glover, Swanson and Spann2013; Jovanovic et al. Reference Jovanovic, Ely, Fani, Glover, Gutman and Tone2013; Acheson et al. Reference Acheson, Geyer, Baker, Nievergelt, Yurgil and Risbrough2015; Gamwell et al. Reference Gamwell, Nylocks, Cross, Bradley, Norrholm and Jovanovic2015; McLaughlin et al. Reference McLaughlin, Sheridan, Gold, Duys, Lambert and Peverill2015; Steiger et al. Reference Steiger, Nees, Wicking, Lang and Flor2015). Following this line of reasoning, a reduced startle potentiation to the danger cue in PTSD in the present study indicates an attenuated differentiation between danger and safety. However, previous findings were heterogeneous regarding to whether an attenuated differentiation is due to a higher response to the safety cue (Grillon & Morgan, Reference Grillon and Morgan1999; Jovanovic et al. Reference Jovanovic, Norrholm, Blanding, Davis, Duncan and Bradley2010; Davis et al. Reference Davis, Jovanovic, Norrholm, Glover, Swanson and Spann2013; Acheson et al. Reference Acheson, Geyer, Baker, Nievergelt, Yurgil and Risbrough2015), and/or lower response to the danger cue (Jovanovic et al. Reference Jovanovic, Ely, Fani, Glover, Gutman and Tone2013; McLaughlin et al. Reference McLaughlin, Sheridan, Gold, Duys, Lambert and Peverill2015). A recent study by Lang et al. (Reference Lang, McTeague and Bradley2016; see also McTeague et al. Reference McTeague, Lang, Laplante, Cuthbert, Shumen and Bradley2010; McTeague & Lang, Reference McTeague and Lang2012) suggested that in general the frequency of traumatisation affects whether startle reactivity is increased or decreased: While single trauma has been linked to increased startle reactivity and this may affect both reactivity towards danger and safety cues (Jovanovic et al. Reference Jovanovic, Norrholm, Blanding, Davis, Duncan and Bradley2010), multiple traumas resulted in a blunted startle reactivity (McTeague et al. Reference McTeague, Lang, Laplante, Cuthbert, Shumen and Bradley2010; McTeague & Lang, Reference McTeague and Lang2012; Lang et al. Reference Lang, McTeague and Bradley2016). Our sample of PTSD participants was characterised by repeated exposure to a variety of trauma types (see Table 1). Thus, our finding of a reduced startle response to the danger cue in PTSD is in agreement with recent literature.
Beyond these alterations in startle reactivity, our data suggest that the certainty in evaluating the risk of the presented cues was altered already during fear acquisition: PTSD patients were slower in response to the safety cue, but faster to the danger cue. In healthy controls, this pattern was reversed. This suggests that PTSD participants are more uncertain regarding the threat information of the safety cue. Altogether, these findings on the differentiation between the danger and safety cue may additionally support alterations in processes linked to the generalisation of fear in PTSD, although similar to the generalisation testing explicit assessments of risk were not affected.
Relationship between alterations in fear acquisition and fear generalisation
Based on the theoretical framework of generalisation, how alterations during fear acquisition might impact fear transfer to a wider range of stimuli is important. Our data suggest that a stronger increase in reaction times during generalisation testing was related to processing during acquisition in PTSD, namely to a lower expectation of risk and a stronger discrimination between CS+ and CS− indicated by FPS. However, this correlation could not be confirmed to be specific for PTSD since comparing the strength of these relationships between groups revealed no statistically significant differences. Moreover, we found that a higher expectation of risk during generalisation testing was related to a higher expectation of risk during fear acquisition and a reduced differentiation in FPS between the safety and danger cues in PTSD. However, the latter alteration affected risk expectations independently of the similarity of stimuli with the danger and safety cues, revealing that they are less relevant for the strength of generalisation.
The impact of childhood maltreatment on fear generalisation
It is important to note, that our data revealed inconclusive findings on the relevance of traumatisation per se. For many of the outcome measures in the different tasks, differences between trauma controls compared with either healthy controls or PTSD participants could not unequivocally be confirmed. On one hand, differences compared to the healthy control group were observed only at a marginally significant level or only without correcting for multiple comparisons (such as an alteration in the slope of the reaction time distribution during generalisation testing). One exception is the slower judgement of risk for the safety cue during fear acquisition, which characterises trauma controls when compared with healthy controls. However, on the other hand, trauma controls could mostly not be distinguished from the PTSD group (such as for the online risk rating or FPS during fear acquisition). This suggests that the TC group may show slight alterations in the direction of the PTSD group; however, this was too weakly expressed to be confirmed statistically either in comparison to the healthy group or the PTSD group.
In summary, alterations in explicit fear responses were indicative for PTSD participants, while hints towards differences in an implicit measurement, e.g. reaction times, were also found in trauma controls. However, these were mostly not unequivocally confirmed by statistical testing and should be interpreted with caution. This is in line with the investigation of the alteration of fear learning with the severity of traumatisation and psychopathology: We found no relation of alterations during generalisation testing, i.e. slope of reaction time distribution and the severity of PTSD symptoms or the severity of childhood traumatisation either within groups or across traumatised participants. These findings differ from previous studies, which linked childhood maltreatment (Morey et al. Reference Morey, Dunsmoor, Haswell, Brown, Vora and Weiner2015), and PTSD symptom severity (Kaczkurkin et al. Reference Kaczkurkin, Burton, Chazin, Manbeck, Espensen-Sturges and Cooper2016) to alterations during generalisation testing. However, both previous studies identified a covariation specifically for neurobiological alteration. This may point to a differential link of the severity of psychopathology and traumatisation with cerebral in contrast to behavioural correlates of alterations in generalisation. Moreover, both studies included PTSD participants with a history of combat exposure. Future studies must address whether the link between the severity of traumatisation and psychopathology may depend on the trauma type, gender and the use of behavioural or biological measures. Thereby, a precise measurement of the type and timing of maltreatment seems to be important since these factors are increasingly recognised as modulating the impact of traumatisation (Teicher & Samson, Reference Teicher and Samson2016).
Limitations
Finally, some limitations of the present study have to be addressed. The observed effects during generalisation testing are restricted to behavioural measurements and were not observable in FPS as a measure closely related to the activation of the amygdala (Davis, Reference Davis2006). One possible explanation might be psychotropic medication in the PTSD group (Table 1, online Supplementary Material S1) since antidepressants, for example, are known to dampen the FPS response, potentially resulting in a floor effect (Arnone et al. Reference Arnone, Horder, Cowen and Harmer2009). However, additional exploratory analyses excluding PTSD patients with psychotropic medication revealed the same pattern of results suggesting that psychopharmacological treatment does not explain our findings. Another explanation may be the occurrence of dissociative symptoms as these are found to be heightened in the aftermath of chronic childhood abuse (e.g. Steuwe et al. Reference Steuwe, Lanius and Frewen2012) and have been shown to be linked to an attenuation of FPS (Ebner-Priemer et al. Reference Ebner-Priemer, Badeck, Beckmann, Wagner, Feige and Weiss2005). Future studies should investigate whether dissociative symptoms during testing may influence FPS modulation during fear generalisation in PTSD.
Importantly, studies investigating generalisation processes in anxiety disorders also did not consistently find overgeneralisation on both physiological and behavioural levels (Lissek et al. Reference Lissek, Rabin, Heller, Lukenbaugh, Geraci and Pine2010, Reference Lissek, Kaczkurkin, Rabin, Geraci, Pine and Grillon2014; Morey et al. Reference Morey, Dunsmoor, Haswell, Brown, Vora and Weiner2015; Ahrens et al. Reference Ahrens, Pauli, Reif, Muhlberger, Langs and Aalderink2016; Kaczkurkin et al. Reference Kaczkurkin, Burton, Chazin, Manbeck, Espensen-Sturges and Cooper2016; for null findings see Greenberg et al. Reference Greenberg, Carlson, Cha, Hajcak and Mujica-Parodi2013; Tinoco-Gonzalez et al. Reference Tinoco-Gonzalez, Fullana, Torrents-Rodas, Bonillo, Vervliet and Blasco2015). Nevertheless, overgeneralisation may constitute a transdiagnostic alteration in fear processing, but further studies are needed to disentangle the different correlates of fear generalisation processes within and between mental disorders.
Finally, one may critically discuss whether the alterations in reaction times solely reflect an increased uncertainty about the association of a specific stimulus with a specific risk of an aversive event. An alternative explanation may be that participants suffering from a mental disorder may differ in the processing of ambiguity per se and not specifically to ambiguity linked to the expectation of an aversive event, i.e. ‘threat ambiguity’ (Lissek et al. Reference Lissek, Kaczkurkin, Rabin, Geraci, Pine and Grillon2014). However, this explanation seems to be less suited to explain our findings, since we found no reaction time differences between groups when participants assessed the similarity of stimuli varying in ambiguity regarding to purely perceptual stimulus features. Similarly, one may speculate whether reaction time differences may be due to a stronger aversion of the participants to making a mistake. While this may contribute to our findings, this aversion seems to be particularly high when judging danger or safety since we found neither a general slowing of reaction times across experimental conditions nor during judgements of perceptual similarity. This suggests that our findings are specific for judging the risk of aversive consequences.
Finally, it must be emphasised that the reported correlations are exploratory analyses of covariations without correction for multiple testing and therefore have to be interpreted with caution until confirmed in future independent studies.
Conclusions
In conclusion, our results demonstrate alterations in generalisation processes of conditioned fear for the first time in a sample of PTSD patients with a history of repeated childhood abuse. As this population is extremely vulnerable to developing a complex pattern of PTSD, it is important to identify factors predisposing or protecting individuals in later life. The present study extends findings regarding alterations in fear memory in PTSD after childhood abuse, as it provides the first experimental data on actual fear transfer, which may contribute to the loss of feeling safe in everyday life.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S0033291717003713
Acknowledgements
This study was supported by a grant from the German Ministry of Education and Research (BMBF). The authors give special thanks to F. Matthaeus and H. Schönbrodt for their assistance with data collection. The authors thank all participants for their collaboration. This study was supported by the German Ministry of Education and Research (BMBF) RELEASE 01KR1303A. S.H., G.K. and J.T. were supported by a scholarship of the SFB 636 International Graduate Program in Translational Neuroscience founded by the German Research Foundation (DFG).
Declaration of Interest
The authors declare that they have no competing interest.
Ethical Standards
Approval was obtained from the independent Ethics Committee of the Medical Faculty Mannheim at Heidelberg University. Reference number: 2013-635 N-MA. All participants provided written informed consent.







